Capsular Contracture
Want To See Real Breast Revision Results?
Before & After Gallery
Be sure to view our breast revision gallery to see real patient results.
Click HereHas the tissue around your breast implants hardened over time? Are your breast implants painful?
Breast augmentation surgery, as with all surgical procedures, is subject to the potential risks of excessive scar formation. The excessive scarring doesn’t happen on the outside of the breasts, but rather in the layer of tissue that surrounds the breast implant, the capsule. The thickened circumferential scarring of the capsule makes it very tight around the implant(s), leading to distortion of the shape of the breast and pain.
Capsular contracture is one of the most frustrating problems – for patient and surgeon alike- after breast implant surgery. The cause of it eluded plastic surgeons for decades and no good treatment options existed until several years ago when Strattice was introduced. Capsular contracture can happen in one or both breasts. It does not matter what type of implant is used – both saline and silicone can be affected. It can happen just weeks after surgery or not until years later, although it typically happens in the first year after surgery. The unpredictability of it and the high recurrence rates are what make it so frustrating to treat.
So, what exactly is Capsular Contracture?
When a foreign body, like a breast implant, is placed in our body, our body responds by creating a thin layer of scar tissue around the object, in a sense to “wall it off”. This layer of tissue around a breast implant is called the CAPSULE. This is a normal process that happens every time we place an implant in the body. The trouble starts when the body doesn’t stop making the scar tissue. As the tissue of the capsule gets thicker and thicker, it actually contracts and tightens around the implant. This can lead to misshapen breasts and eventually pain. Patients will sometimes remark that their implants got hard. It’s not the actual implant that hardens, but rather the tissue surrounding it.
We have a scale for the severity of Capsular Contracture. It’s called the Baker Scale.
Grade IV
Grade III
Moderate capsular contracture. The breast is firm, and it is visibly misshapen, and often higher than the other side.
Grade II
Mild capsular contracture. The breast has some firmness but looks normal.
Grade I
No evidence of capsular contracture. The breast is soft and looks and feels normal.
What causes Capsular Contracture to happen?
The laying down of the excessive scar tissue is caused by the immune system, but we don’t exactly understand what triggers it. It is thought to be an inflammatory response, and once it’s activated, it’s almost impossible to stop. We have identified several factors that increase your risk for developing capsular contracture:
- Rupture or leakage of a silicone gel implant
- Bacteria on the implant surface. This can come from the skin during surgery, from using the periareolar incision, or from placing the implants in the sub-glandular position. The implant can also get “seeded” with bacteria later if the patient gets a serious bacterial infection or mastitis of the breast.
- Breast infection
- Hematoma or bleeding around the implant. Blood is very inflammatory and causes more scar tissue to form.
- Trauma to the breast
- Smoking causes decreased oxygen in the blood, which can delay healing and increase the risk of infection
- Radiation for cancer treatment
What do I do if I think I have Capsular Contracture?
You should contact your surgeon immediately. Some medications like high dose Vitamin E, antibiotics and Singular have shown some promise in slowing down the inflammatory process. The mainstay of treatment is surgical.
Dr. Gordon & Dr. Reid’s first step in managing capsular contracture is trying to identify the specifics of the first operation or any other factors in the post-operative period, which may have led to its initial development. Often times, a revisionary surgery that changes some of the variables of the previous surgery will be successful, such as a pocket change. We know that placing the implants below the muscle decreases the risk of capsular contracture. We also know that the IMF or Infra-Mammary Fold incision (in the lower breast crease) has the lowest incidence of capsular contracture. For your revision, the options we recommend are the ones that are published in the plastic surgery literature as having the lowest chance of recurrence.
All operations to treat capsular contracture involve removing the scarred capsule and exchanging the implant. Just because the capsule is removed in its entirety doesn’t mean it won’t recur. Remember, it’s an inflammatory process, which is microscopic.
Capsulectomy – refers to removing the entire capsule surgically and changing the implant. Depending on the cause and severity, the recurrence rate can be as high as 50% because once you’ve had capsular contracture, you are more likely to have it again.
Are there any other things I can do to minimize my recurrence risk?
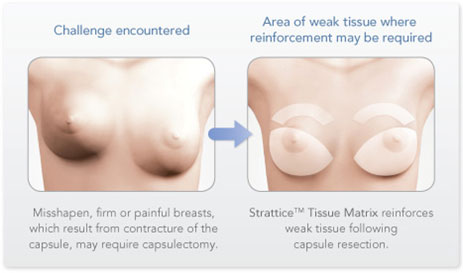
Yes, make Strattice a part of your revisionary surgery! Dr. Gordon & Dr. Reid feel that Strattice has really been a game changer in the treatment of capsular contracture. A large percentage of their practice is revisionary breast surgery, and the use of Strattice has decreased the recurrence rate to less than 5%.
Strattice is an Acellular Dermal Matrix or ADM that has been used for many years in breast cancer reconstruction. It’s a piece of tissue that can be used in a variety of different ways to provide support to the breast tissue and skin. As plastic surgeons started using Strattice in a variety of applications, we noticed that we weren’t seeing as many patients with capsular contracture. Studies were done, and we learned that Strattice reduces the risk of capsular contracture by altering the body’s scarring mechanism around the implant. When we look at the capsule-Strattice interface under the microscope, we see that the capsule will grow to the edge of the Strattice, but it can’t grow across it. The only way that the capsule can contract is when it completely encircles the implant. The Strattice halts the capsule in its tracks, and prevents capsular contracture. The other neat thing is the Strattice eventually gets replaced with your own cells and collagen. It literally becomes a part of you. As the term, acellular dermal matrix implies, the Strattice acts as a scaffold for your own cells to populate and make collagen. Another material called Seri was approved last year and clinical results are similar in reducing the capsular contracture.
Where is the Strattice or Seri placed?
The Strattice or Seri is usually sutured in place to the lower edge of the pectoral major muscle down to the level of the fold to give complete coverage over the implant.
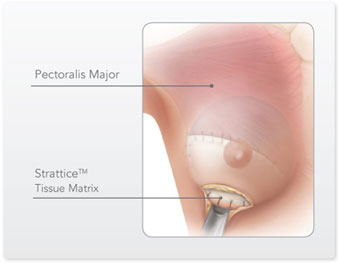
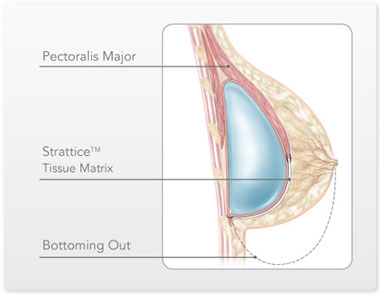
FAQ’s on Strattice
Every patient is unique, so we are thrilled to have breast revision experts, Dr. Gordon and Dr. Reid, for these challenging revision cases. Call today 512.371.8817 to schedule your consultation to discuss your concerns and revision options.